The link between the heart and the brain has been known for several centuries by examples such as syncope or death from extreme emotions and stressors.
Emerging research has provided new insights into pathogenic role of the deregulation of the heart-brain axis (HBA), a bidirectional flow of information, in leading to severe multiorgan disease syndrome (MODS) in patients with confirmed infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2).
In-depth characterisation of heart-brain communication in critically ill patients with severe acute respiratory failure is attracting significant interest in the COronaVIrus Disease 19 (COVID-19) pandemic era during intensive care unit (ICU) stay and after ICU or hospital discharge.
What is the Heart-Brain Axis?
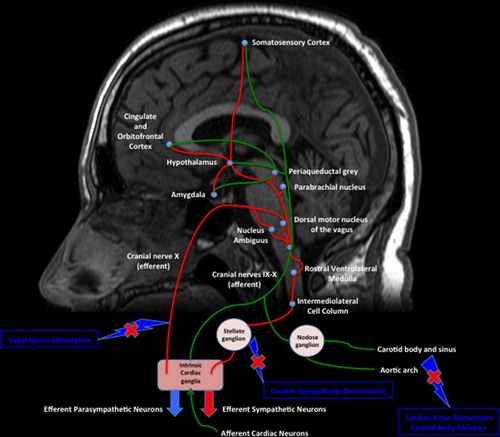
Clinical studies of both animals and humans have illustrated a complex network of cortical and subcortical regions involved in processing and control of the cardiovascular function.
This network involves several highly interconnected cortices, subcortical forebrain structures (including the amygdala and the hippocampus), and brain stem areas (including the hypothalamus, the bed nucleus of the stria terminalis, the periaqueductal gray, the parabrachial region, and the ventrolateral medulla). Higher cortical areas, including the orbitofrontal cortex and the dorsal cingulate cortex, process the afferent information ascending from the periphery and other brain areas and modulate the efferent autonomic outflow to adjust the cardiovascular function.
How The Response Works
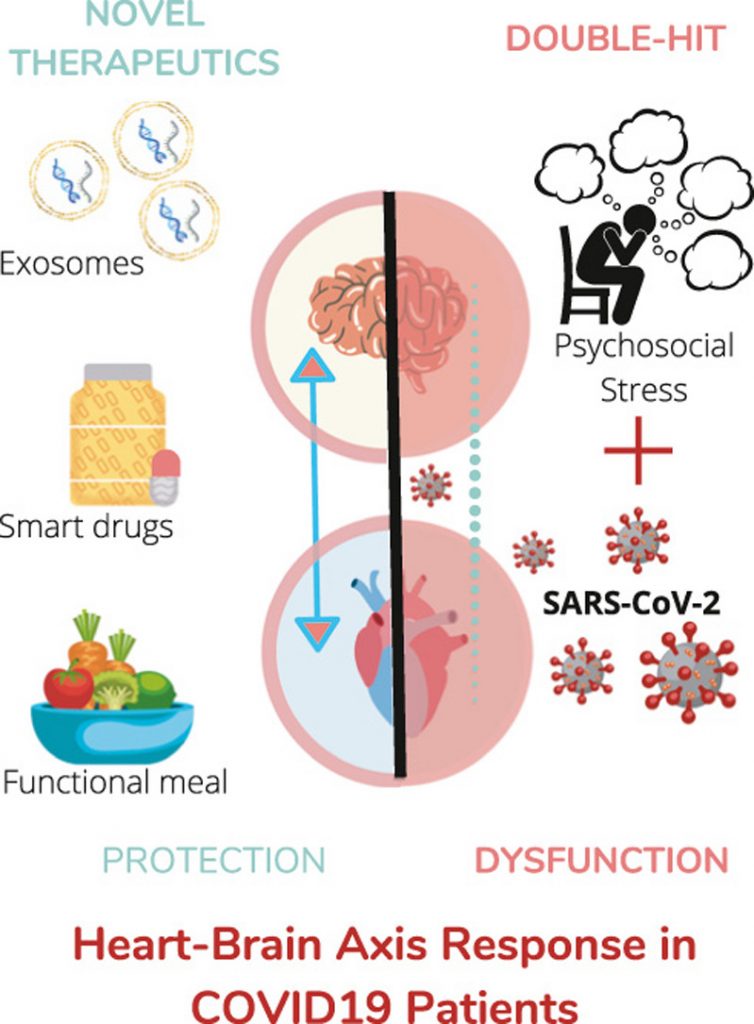
Key Highlights of Research
SARS-CoV-2 may interfere with HBA either through direct neurotropism either through direct endothelial injury.
Dysregulated heart-brain axis (HBA) may contribute to severe multiorgan disease syndrome (MODS) in COVID-19 patients.
Definition of HBA disorders in COVID-19 patients will help to personalise pharmacological and non-pharmacological treatments.
References:
Website: https://www.sciencedirect.com/science/article/abs/pii/S1043661821001651#keys0005
Website: https://www.ahajournals.org/doi/full/10.1161/circresaha.116.308446
